REDUCTION PHASE VS MAINTENANCE PHASE OF COMPRESSION: KEEPING THE BALANCE
- Catharine Burt RN, BScN, RMT, CDT
- Sep 19, 2021
- 4 min read

Compression, skin care, exercise and manual lymphatic drainage treatments are the four pillars of lymphedema treatment. The different modalities work together to reduce skin and tissue hardening, improve lymphatic and venous circulation and either reduce or maintain limb size.
When it comes to swelling, the use of compression is vital not only to reducing the size of limb, but also in maintaining its size.
There are two different phases of compression therapy:
1) THE REDUCTION PHASE, which is used to reduce limb size, soften hard tissue, stop any weeping or fluid leakage, and prevent skin breakdown, infection and loss of mobility. In this phase short stretch material is used to apply pressure to the limb that aids in swelling reduction. When reducing a limb for the first time the short stretch reduction system is worn 23 hours a day and removed only for hygiene and skin care purposes. There are a few different methods for reducing swelling used today:

Short stretch bandages applied in layers over foam padding has been the mainstay of reduction phase therapy for decades. It is an economical method of swelling reduction and self-bandaging is a tool that everyone should have in their “lymphedema maintenance tool-box”. Watch for an upcoming blog on this topic

Adhesive bandage systems are available that can stay on
For up to 7 days. While they are expensive and do not allow for daily skin self-assessment and care they are much less bulky and provide allowances for footwear and clothing better than the bulky multi-layered short stretch bandages and foam as above. Typically, you would not apply these by yourself and so frequent visits to a trained and qualified health professional would be in order. In the intensive phase, this type of bandage system is usually changed every 2 to 3 days as the size of your limb reduces.

Velcro style garments are now being used as reduction tools. They are a less bulky option to the multi-layer bandaging system but are bulkier than the adhesive bandage systems. They are adjustable so that if one area is too tight and causing discomfort you can just loosen it as opposed to unwrapping the short stretch bandages to find the cause and then re-wrap again or completely removing the adhesive style and having to wait to get them re-applied. Garment company studies have shown good results in reducing the size of a limb. This may look easy, but some people will require help to get the correct tension and placement of the garment pieces.
FACTORS THAT YOU SHOULD CONSIDER WHEN CHOOSING A REDUCTION OPTION
TIME
a) It takes longer to apply the multi-layer bandage systems than it does to put on a Velcro garment. However, if you learn to self-bandage, the frequency of visits with your professional may be reduced (optimally, you would be receiving treatment by a lymphedema therapist daily regardless of the reduction method, but this is usually not financially feasible in areas where treatment is not covered by health plans).
b) The adhesive bandage systems are not usually self-applied. Therefore, you would need to arrange for a specialist to apply them and have the time to visit them on a frequent basis. Not all lymphedema therapists have training in the application of this method so if this method is your choice, you may have to travel to a therapist who has the training.
MOBILITY
a) It is wise to think about whether you have the ability to bend, stoop and reach when thinking about which method you will be choosing.
b) Those with arthritis or nerve related disruptions in their joints or hands may find one method easier than another.
c) Bulkier systems may affect the footwear you can get around in. Additionally, you may want to consider how much these systems will affect your movement capability when choosing which you would prefer.
COST
In order from least to most expensive over the course of reduction phase (4-6 weeks):
a) Short stretch bandage systems
b) Velcro style garments
c) Adhesive bandage systems
OTHER THINGS TO CONSIDER:
i) Velcro systems are washable and re-usable. Most companies will say that they will be effective for up to 6 months. Therefore, can be tucked away when done your initial reduction phase for possible future use.
ii) Short stretch bandages are washable and re-usable and can also be tucked away for future use after the initial reduction phase is complete. If foam is used as an underpadding it should last the 4–6-week time period of initial reduction. The only thing you may need to replace is the toe or finger gauze if used in the process.
iii) Adhesive bandage systems are used once and discarded requiring new every time the bandages are changed.
2) THE MAINTENANCE PHASE
When the reduction phase is finished, compression is needed to maintain the size and shape of the limb. Compression garments help keep tissue soft and aid in fluid return from the tissues to the lymph and vascular systems. See my blog on knowing your compression needs and compression: medicine for your lymphedema for more information.
A variety of different compression garments are available for the maintenance phase to suit your needs, colour and pattern preferences. Your certified lymphedema specialist fitter can help you with these choices.
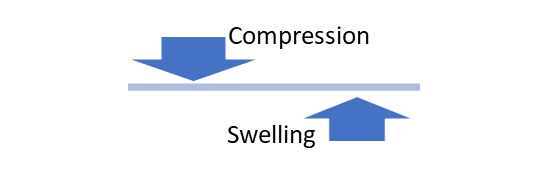
KEEPING THE BALANCE

Our bodies are susceptible to many forces that can increase swelling and disrupt the balance.
Here are a few:
a) Increasing age
b) Infection
c) Conditions of inflammation such as arthritis
d) Injury/trauma or surgery
e) Increased heat and humidity
f) Weekend warrior exercise
g) Medications
h) Other medical conditions
i) Diet and reactions to ingredients in foods
j) Increased weight
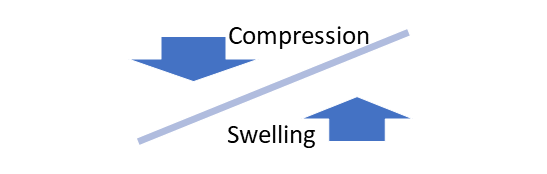
THE MAINTENANCE PHASE CAN BE A ROLLERCOASTER WHERE YOU ARE ALTERNATING BETWEEN THE REDUCTION AND THE MAINTENANCE PHASES
There may be times after entering the maintenance phase that you may have to begin another reduction phase. There may be times that you want to bandage or use your Velcro garment overnight as a temporary reduction solution. Keeping the balance of fluids out of your tissues requires you to be vigilant about your compression. If you notice your limb swelling into your garment as the day goes on—you need to have your garment assessed—is it too old? Is it not enough compression? Is the fabric stiffness enough? Do you need to see your doctor?